Assessing the Prevalence of Latent Tuberculosis Infection in Healthy and Immunocompromised Individuals in Dutsin-Ma Metropolis, Katsina State, Nigeria
A Cross-Sectional Study
DOI:
https://doi.org/10.5281/zenodo.15777259Abstract
 Abstract Views: 197
Abstract Views: 197
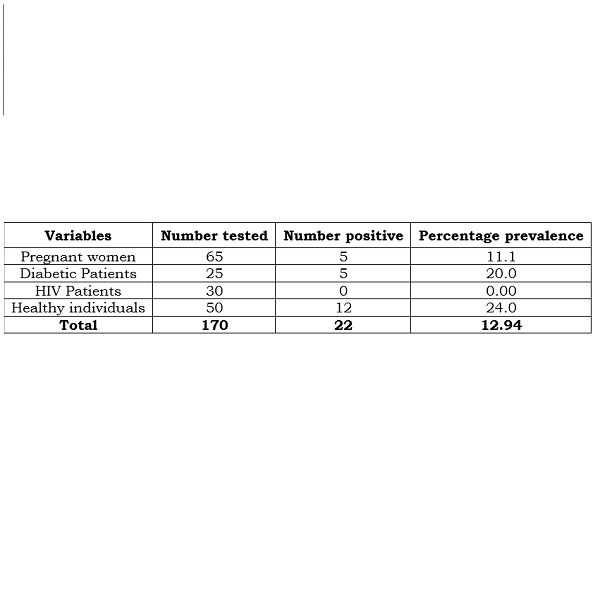
Latent Tuberculosis Infection (LTBI) is a widespread condition affecting a significant portion of the global population. People with LTBI have a 5-10% chance of developing active Tuberculosis (TB) during their lifetime. However, there is a shortage of data on the prevalence of LTBI in healthy and immunocompromised individuals in the Dutsin-Ma metropolis. Identifying and treating LTBI is crucial for reducing the burden of TB globally. This cross-sectional study aimed to determine the prevalence of LTBI in healthy and immunocompromised patients in the Dutsin-Ma, Katsina State, Nigeria. 170 blood samples were randomly collected from participants across three (3) healthcare facilities in Dutsin-Ma in September 2023 and screened for anti-TB antibodies using the Rapid Tuberculosis Test Card™ (RTTC); 50 were healthy participants, 65 were pregnant women, 30 were HIV-positive patients, and 25 were diabetic patients. The sociodemographic data were collected and analyzed using descriptive statistics and Chi-square to test for association. Among the 170 participants tested, 12.94 % (22/170) were serologically positive for anti-TB antibodies. Several risk factors associated with LTBI were identified. However, statistically, there was not enough evidence to conclude that any of the risk factors are significantly associated with the prevalence of LTBI at 95% CI and a P-value of ≤ 0.05 in this survey. The study highlights the need for routine screening and treatment of LTBI in both healthy and immunocompromised individuals in the study locality. This is vital in reducing the global burden of LTBI and active TB infections.
Keywords:
Diabetes mellitus, Dutsin-Ma, Human immunodeficiency virus, Immunocompromised, Latent tuberculosis, Rapid tuberculosis test cardReferences
Akinshipe, B. O., Yusuf, E. O., Akinshipe, F. O., Moronkeji, M. A., & Nwaobi, A. C. (2019). Prevalence and determinants of pre-diabetes and latent tuberculosis infection among apparently healthy adults in three communities in Southern Nigeria. International Journal of Immunology, 7(2), 23-32.
Alene, K. A., Viney, K., Moore, H. C., Wagaw, M., & Clements, A. C. (2019). Spatial patterns of tuberculosis and HIV co-infection in Ethiopia. PloS one, 14(12), e0226127. https://doi.org/10.1371/journal.pone.0226127
Al-Rifai, R. H., Pearson, F., Critchley, J. A., & Abu-Raddad, L. J. (2017). Association between diabetes mellitus and active tuberculosis: A systematic review and meta-analysis. PloS one, 12(11), e0187967. https://doi.org/10.1371/journal.pone.0187967
Bloom, B. R., & Murray, C. J. (1992). Tuberculosis: commentary on a reemergent killer. Science, 257(5073), 1055-1064. https://doi.org/10.1126/science.257.5073.1055
Chen, Z., Wang, T., Du, J., Sun, L., Wang, G., Ni, R., ... & Gong, W. (2025). Decoding the WHO Global Tuberculosis Report 2024: A Critical Analysis of Global and Chinese Key Data. Zoonoses, 5(1), 999. https://doi.org/10.15212/ZOONOSES-2024-0061
Chukwudi, U. K., Chuka, E. P., & MaryAnn, O. N. (2020). Interferon gamma release assay of latent tuberculosis infection amongst prisoners in Anambra State. IOSR Journal of Dental and Medical Sciences, 19, 10:11. https://doi.org/10.9790/0853-1910110715
Churchyard, G. J., Scano, F., Grant, A. D., & Chaisson, R. E. (2007). Tuberculosis preventive therapy in the era of HIV infection: overview and research priorities. The Journal of infectious diseases, 196(Supplement_1), S52-S62. https://doi.org/10.1086/518662
Corbett, E. L., Marston, B., Churchyard, G. J., & De Cock, K. M. (2006). Tuberculosis in sub-Saharan Africa: opportunities, challenges, and change in the era of antiretroviral treatment. The Lancet, 367(9514), 926-937. https://doi.org/10.1016/S0140-6736(06)68383-9
Dixon, B. (2007). Diabetes and tuberculosis: an unhealthy partnership. The Lancet Infectious Diseases, 7(7), 444. https://doi.org/10.1016/S1473-3099(07)70144-5
Firănescu, A. G., Popa, A., Sandu, M. M., Protasiewicz, D. C., Popa, S. G., & Moță, M. (2016). The global prevalence and incidence of diabetes mellitus and pulmonary tuberculosis. Romanian Journal of Diabetes Nutrition and Metabolic Diseases, 23(3), 319-326.
Gazette, N. O. (2009). Nigeria census final results. Official Gazette, National Population Commission Federal Republic of Nigeria.
Gounder, C., de Queiroz Mello, F. C., Conde, M. B., Bishai, W. R., Kritski, A. L., Chaisson, R. E., & Dorman, S. E. (2002). Field evaluation of a rapid immunochromatographic test for tuberculosis. Journal of clinical microbiology, 40(6), 1989-1993. https://doi.org/10.1128/jcm.40.6.1989-1993.2002
Harries, A. D., Satyanarayana, S., Kumar, A. M. V., Nagaraja, S. B., Isaakidis, P., Malhotra, S., ... & Kapur, A. (2013). Epidemiology and interaction of diabetes mellitus and tuberculosis and challenges for care: a review. Public health Action, 3(1), 3-9. https://doi.org/10.5588/pha.13.0024
Hino, Y., Eshima, N., Tokumaru, O., Bacal, K., Tanaka, Y., Karukaya, S., & Yamashita, Y. (2022). A change in the timing of the Bacillus Calmette–Guérin vaccination in 2013 was associated with an increase in the incidence rate of infants with latent tuberculosis infection. Journal of Infection and Chemotherapy, 28(7), 929-933. https://doi.org/10.1016/j.jiac.2022.03.018
Lyashchenko, K. P., Singh, M., Colangeli, R., & Gennaro, M. L. (2000). A multi-antigen print immunoassay for the development of serological diagnosis of infectious diseases. Journal of immunological methods, 242(1-2), 91-100. https://doi.org/10.1016/S0022-1759(00)00241-6
Migliori, G. B., Ong, C. W., Petrone, L., D'Ambrosio, L., Centis, R., & Goletti, D. (2021). The definition of tuberculosis infection based on the spectrum of tuberculosis disease. Breathe, 17(3). https://doi.org/10.1183/20734735.0079-2021
Morrison, J., Pai, M., & Hopewell, P. C. (2008). Tuberculosis and latent tuberculosis infection in close contacts of people with pulmonary tuberculosis in low-income and middle-income countries: a systematic review and meta-analysis. The Lancet infectious diseases, 8(6), 359-368. https://doi.org/10.1016/S1473-3099(08)70071-9
Orazulike, N. C., Alegbeleye, J. O., Obiorah, C. C., Nyengidiki, T. K., & Uzoigwe, S. A. (2017). A 3-year retrospective review of mortality in women of reproductive age in a tertiary health facility in Port Harcourt, Nigeria. International journal of women's health, 769-775. https://doi.org/10.2147/IJWH.S138052
Pesanti, E. L. (1994). The negative tuberculin test. Tuberculin, HIV, and anergy panels. American journal of respiratory and critical care medicine, 149(6), 1699-1709. https://doi.org/10.1164/ajrccm.149.6.7710481
Raviglione, M. (2006). XDR-TB: entering the post-antibiotic era?. The International Journal of Tuberculosis and Lung Disease, 10(11), 1185-1187.
Say, L., Chou, D., Gemmill, A., Tunçalp, Ö., Moller, A. B., Daniels, J., ... & Alkema, L. (2014). Global causes of maternal death: a WHO systematic analysis. The Lancet global health, 2(6), e323-e333. https://doi.org/10.1016/S2214-109X(14)70227-X
Van Rie, A., & Enarson, D. (2006). XDR tuberculosis: an indicator of public-health negligence. The Lancet, 368(9547), 1554-1556. https://doi.org/10.1016/S0140-6736(06)69575-5
Vynnycky, E., & Fine, P. E. (2000). Lifetime risks, incubation period, and serial interval of tuberculosis. American journal of epidemiology, 152(3), 247-263. https://doi.org/10.1093/aje/152.3.247
World Health Organization. (2022). Global tuberculosis report 2021: supplementary material. World Health Organization.
World Health Organization. (2024). WHO operational handbook on tuberculosis. Module 1: prevention-tuberculosis preventive treatment. World Health Organization.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 Biomedicine and Chemical Sciences

This work is licensed under a Creative Commons Attribution 4.0 International License.



















